
Patient Case Study: Madeline Hawkins
Madeline Hawkins was diagnosed with Chronic Myeloid Leukaemia (CML) back in June 2012 after she was referred for additional blood tests following complains of pain in her feet.
Johanna Greenaway is hugely positive about the impact of participating in a blood cancer clinical trial.
Put simply: “It made a huge difference to my quality of life”.
Retired Johanna, 78 from Caerphilly in Wales, was diagnosed with Chronic Lymphocytic Leukaemia (CLL) in 2009 and didn’t have any symptoms when she faced the news, however.
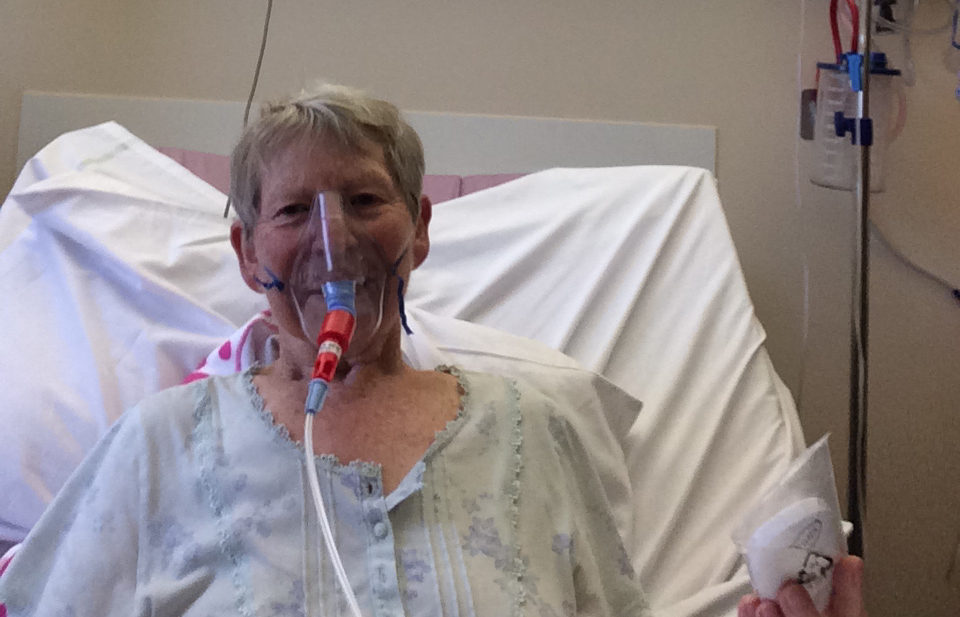
She said: “I was diagnosed after a blood test was taken because of a reaction to some medication. I did not have any symptoms.
“At the time of the diagnosis, because I was so shocked, the consultant asked if I understood what it meant. I didn’t, because I felt well and didn’t know that there were so many kinds of leukaemia.”
The initial approach, as in so many cases, was “watch and wait” – although she admits it was more like “watch and worry”.
She continued: “I was surprised when the consultant said that I would not be having any treatment at the moment because it was not beneficial to have treatment too early.

“That was very surprising and concerning. He said we do “watch and wait”. Many people consider that to be watch and worry!
“For the next five years I keep quite well but did have frequent ear infections, which were treated with antibiotics and also chest infections. Eventually it was decided to put me on a monthly immunoglobulin infusion to help my immune system. The chest infections got quite bad and in November 2013 I was admitted to hospital with pneumonia. I was there for about 3 weeks. I was very weak when I came out and was not making very good progress with the various medications.”
That’s when Johanna’s story took a positive turn.
She was transferred to the care of Professor Christopher Fegan at Trials Acceleration Programme (TAP) centre – the University Hospital of Wales in Cardiff.
He told her that fresh hope – in the shape of a new clinical trial called IciCLLE – may be at hand.

She continued: “Professor Fegan said that chemotherapy wasn’t an option for me. But he was involved in research into CLL and knew that there were trial preparations taking place with Ibrutinib, which was not a chemotherapy medication. He was waiting for it to be released and hoped to get me on that.
“Early in September 2014, he rang me at home to say that the trial details had been released and asked if I’d be interested in taking part.
“I decided I would and signed up for it. It was for 40 patients in the UK – so I am one of them.
“Once I started on the medication it soon started to help my condition improve. My spleen had become quite large, and I felt very, very tired.
“The medication made a huge difference to my quality of life. I put on some of the weight I had lost and had a lot more energy. Not as much as I used to have but, still, it gave me back some – and I was able to attend some of the activities I was used to, albeit in a more back seat role.”
Fast forward to 2021 and she still has check-ups and couldn’t speak highly enough of those who treat her at the Welsh TAP centre.
She added: “I am seen regularly at the Clinical Research Unit at the U.H.W. who are like family friends now. They are so understanding and caring – always ready to help if I have a problem.”


Madeline Hawkins was diagnosed with Chronic Myeloid Leukaemia (CML) back in June 2012 after she was referred for additional blood tests following complains of pain in her feet.

Patient/caregiver volunteers required to support a clinical trial proposal for patients with AML